Prophylactic Double Mastectomy: Surgery Day
While I was so certain about my reason to have the prophylactic double mastectomy, fear of the unknown was my biggest obstacle on surgery day.
If anyone asked how I was feeling about my upcoming surgery the one phrase I that I always said “I’m at peace”.
**This post contains talk about surgery and pictures that could make you queasy, read with caution.**

I knew in my heart of hearts that this was THE best decision for myself, my girls, and my husband.
That I could be proactive and greatly reduce my risk of getting breast cancer due to my genetic mutation CHEK2, instead of reactive, because it was a matter of “when” not “if” I would get breast cancer.

Yet there I was the night before my surgery, the morning when the doctor stepped foot in my room to say hello before surgery, and while they were putting me under… crying.
Courtney kept saying that I didn’t have to do anything I didn’t want to do, and while I knew backing out was always an option, I knew it wasn’t the right option.

My surgery day team.
This is one of the times where I am grateful that my husband, Courtney, is a physician assistant and works in the same hospital where I am having my surgery.

Not only does he know both my breast surgeon and plastic surgeon, we are also friends with several of the nurses, anesthesia, and other key parts of the medical team at the hospital.

I was very fortunate to have one of my friends and old neighbor, Jeanne, be my pre-op nurse. I cannot even begin to tell you how much that settled my nerves.

Post surgery, and while I vaguely remember seeing her, I was blessed to have another nurse friend,Kelly, take care of me when I went into recovery.
I know this is something that is not typical, but definitely something that I do not take for granted.
My best advice, when you do decide to have a prophylactic double mastectomy, or any procedure for that matter, ask around and get opinions from other people on who to go to or who to avoid.
The surgery game plan.
What would take hours, the surgeon explained for me, would feel like 5 minutes.
The surgeon assured Courtney they would call every half hour or so keeping him posted on each step of the surgery.
Remove the tissue from one breast, call.
Remove the tissue from the other breast, call.
Check for blood flow, call.
The plastic surgeon would do her part, they would call.
After my breast surgeon left, the plastic surgeon came in and we went over my desire to keep my nipples and if possible, move my breasts up a bit.
We also went over the possibility of going to expanders instead of implants, but that no matter what a second procedure would be needed in the reconstruction to do fat grafting.
Since all the breast tissue is removed the expanders/ implants would fill the space, but would have ripples and the fat grafting (taking fat from other parts of your body and placing inside the breasts) would smooth everything out.
The plastic surgeon used her surgical marker to map out her route and symmetry.
My new best friend has entered the room.
Shortly after the breast doctor and plastic surgeon left, my most favorite team walked in, anesthesia.
After joining one of the mastectomy support groups on FB, anesthesia was one of the hot topics and key to as pain free of a recovery as possible.
The anesthesiologist worked his magic and inserted catheters in my back, which would later hold my On-Q pain pumps. (This wasn’t anything special for me, this is standard care for this type of surgery.)

He also gave me something to help with my nerves and I felt more calm than ever.
Of course the anesthesiologist was there during the surgery to monitor me during the entire 7 hours.
Rolling into the operating room and waking up
This is where things get really fuzzy.
I barely remember being rolled into the operating room and getting on to the operating table.
The breast surgeon was to my right and she pointed out one of her nurse practitioners I’ve seen many times before who was also in the room.
As the surgeon held my hand and told me she would take care of me, the oxygen mask placed on me and the next thing I hear is “she’s awake”.
Later Courtney would tell me the surgery took 7 hours and I took another hour to wake up in recovery.
They were starting to become concerned because of how long I was taking to wake up and were going to try something to help wake me up when I finally woke up on my own.

(Let’s be honest, I haven’t slept well in 15 years so the anesthesia nap is very much welcomed. 😉 )
When I woke up they told me I did keep my nipples, but that because one breast was a whole cup size bigger than the other and there was one small area of concern for blood flow, they felt expanders would be a better option than going direct to implant.
Even coming out of anesthesia I was awake enough to understand and I was slightly bummed.
Road to healing
My surgery was considered outpatient, but I did spend on night in the hospital.
I was still pretty out of it because of anesthesia and all the medication, but I was surprised that I wasn’t so much in pain as I just felt sore like I did a big chest day at the gym.
My nursing staff was truly the best and were very attentive to my needs, which really wasn’t much because all I pretty much did was sleep.

Aside from the nice water bottle with straw, which is key because I wasn’t allowed to move my arms above elbow level, there was also a package that contained a face mask and ear plugs.
And trust me, I used them.
Naturally I slept too well and the nurse had to wake me up every time she had to come in to check my vitals or give me meds.
I truly left the hospital pretty refreshed considering the extensive surgery I just had.
Heading home
I wore the clothes I came in with that included comfy pajama bottoms, a zip up hoodie, and flip flops.

They placed me in a surgery bra and helped me into a surgical camisole that had pockets inside for the drains.
I ended up with two drains that come out on both sides right under where the natural bra line would be.
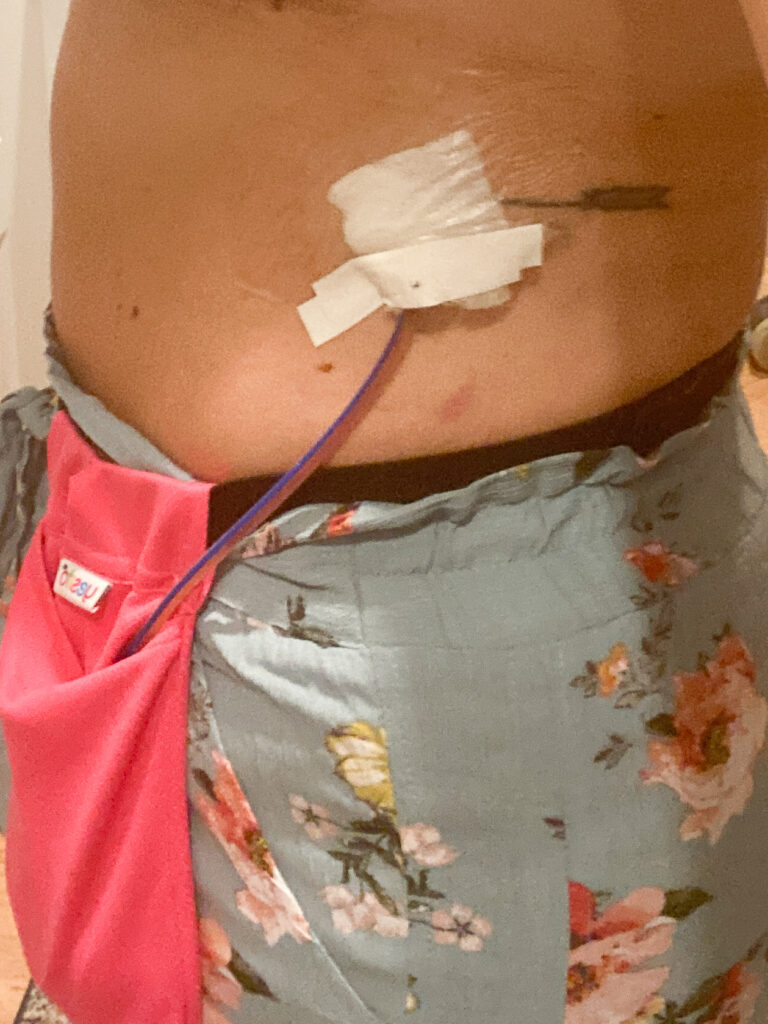
Before I went home the doctor came in to see me and that was the first time I got to see what everything looked like.
Going into surgery I was pretty busty, so to see the very bruised, lumpy, and very deflated chest that was now mine, was a lot to take in.
On the other hand, this is where the next step of the journey would begin and I felt a lot more at peace knowing that my chances of getting breast cancer were drastically reduced.

Once the physical therapist came in to give me exercises I needed to do and watched me get up and walk around, I was released to go home.
Final thoughts
Making such a huge decision took months of research, speaking with many medical professionals, and of course talking to my family.
I knew in my heart of hearts that this was the best decision for me and my future, but it was still scary not knowing how things would turn out.
Being on this side of surgery I would do it again and I plan on staying in the online support groups to help future women like me who will be faced with this same decision.
I realize now that what once seemed like a very extreme decision is actually more common than I ever knew.
As I type this I’m exactly three weeks out from surgery and I’m glad that I started with expanders, the pain truly stayed away thanks to the pain pumps and staying on top of my meds, and I’m very excited for the future.

Let's connect!!
Stay connected for all your DIY and organizing needs!





